The Dysphagia Expert
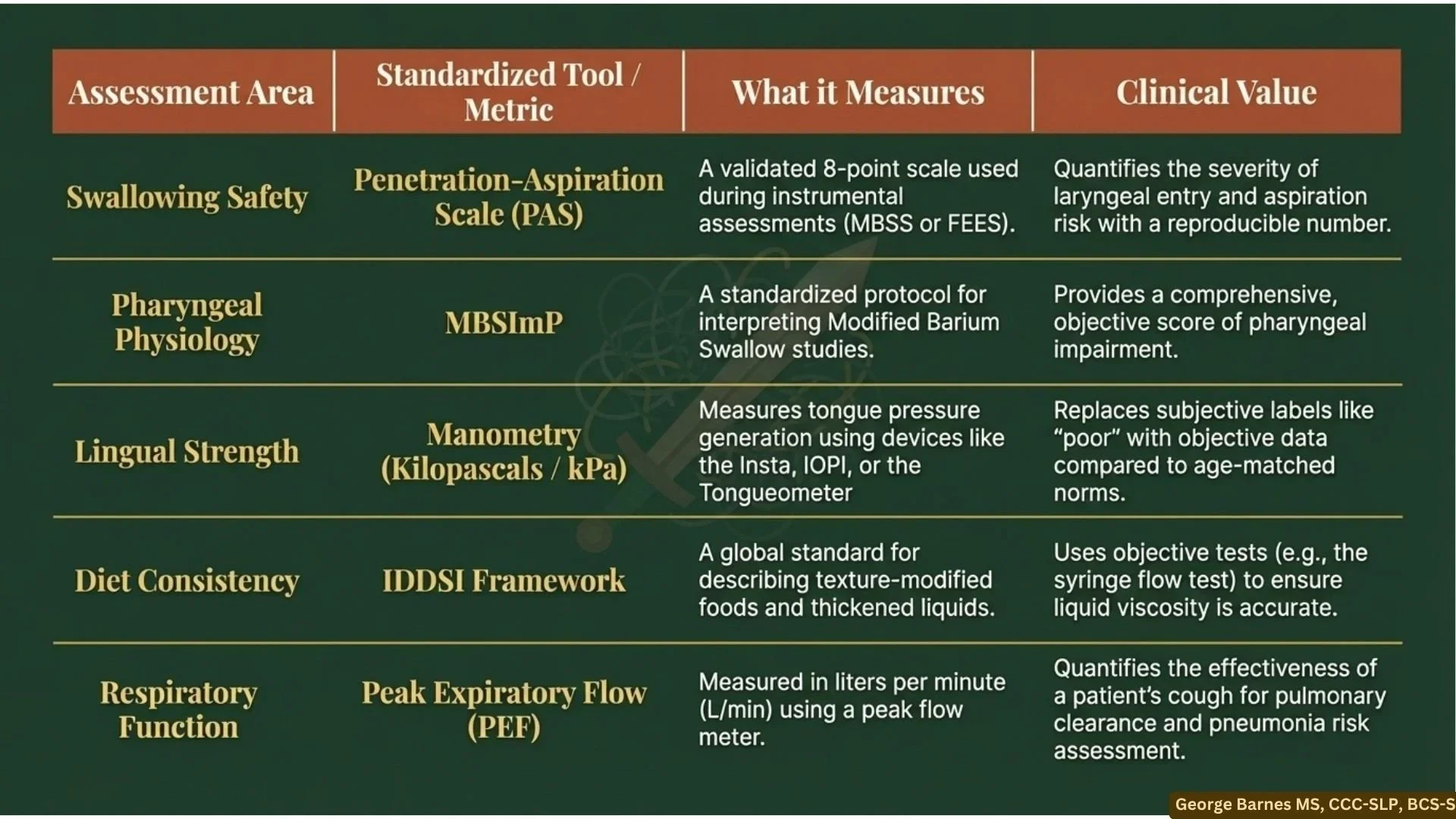
Standardization: Why the future of medical speech pathology depends on it.
Subjective guessing leaves dysphagia patients vulnerable. Discover why the future of medical speech pathology depends on standardizing your practice with objective data. Includes a free downloadable guide.

The Modified Barium Swallow Study: So much more than a pass/fail test
The MBSS is a physiological evaluation, not a simple pass or fail. Learn why standardizing IDDSI, Varibar, and protocols like MBSImP is vital for accurate dysphagia diagnosis, patient safety, and meeting CMS expectations.

Breathing and Swallowing: What you need to know
Learn how respiratory status, tachypnea, and high-flow oxygen impact swallowing safety. Explore clinical strategies for managing dysphagia in medically complex patients.

Treating the Person, Not the Swallow: A case study on impulsivity and quality of life
Explore a clinical case study on dysphagia, impulsivity, and the Hawthorne Effect. Learn why treating the person is more important than the swallow study results.

Palliative Care: What can the SLP do when “fixing” the swallow is no longer possible?
Discover how Speech-Language Pathologists transition from rehabilitation to comfort-based care. Learn about palliative vs. hospice care, spaced retrieval for dementia, and person-centered goals for swallowing and dignity.

The Magic Mirror: And a potential code to swallowing success
Discover how biofeedback tools like sEMG and tongue manometry act as a "magic mirror" for dysphagia rehabilitation, helping SLPs and patients visualize progress and improve swallowing outcomes.

Parkinson’s and Dysphagia: What you need to know
Understand the critical link between Parkinson’s and swallowing difficulties. Learn the warning signs of dysphagia and what interventions work best.

4 Ways Medications Impact Swallowing
While we often link dysphagia to neurological injury, "harmless" pills can be the hidden culprit. Discover 4 ways medications—from antihistamines to CNS depressants—impact saliva, motor function, and GI motility, and why SLPs must look beyond the swallow in a vacuum.

Don’t Get Pinched: How to Spot "Crabby" Research
Protect your clinical practice from misinformation. Learn how to use the CRABS mnemonic to evaluate dysphagia research, spot "snake oil" on social media, and ensure your patient care is strictly evidence-based.

Curing the Chronic Cough
Is your patient struggling with a cough that won't stop despite clear lung scans? Learn how Behavioral Cough-Suppression Therapy retrains your nervous system to stop the cycle of refractory chronic cough without medication.
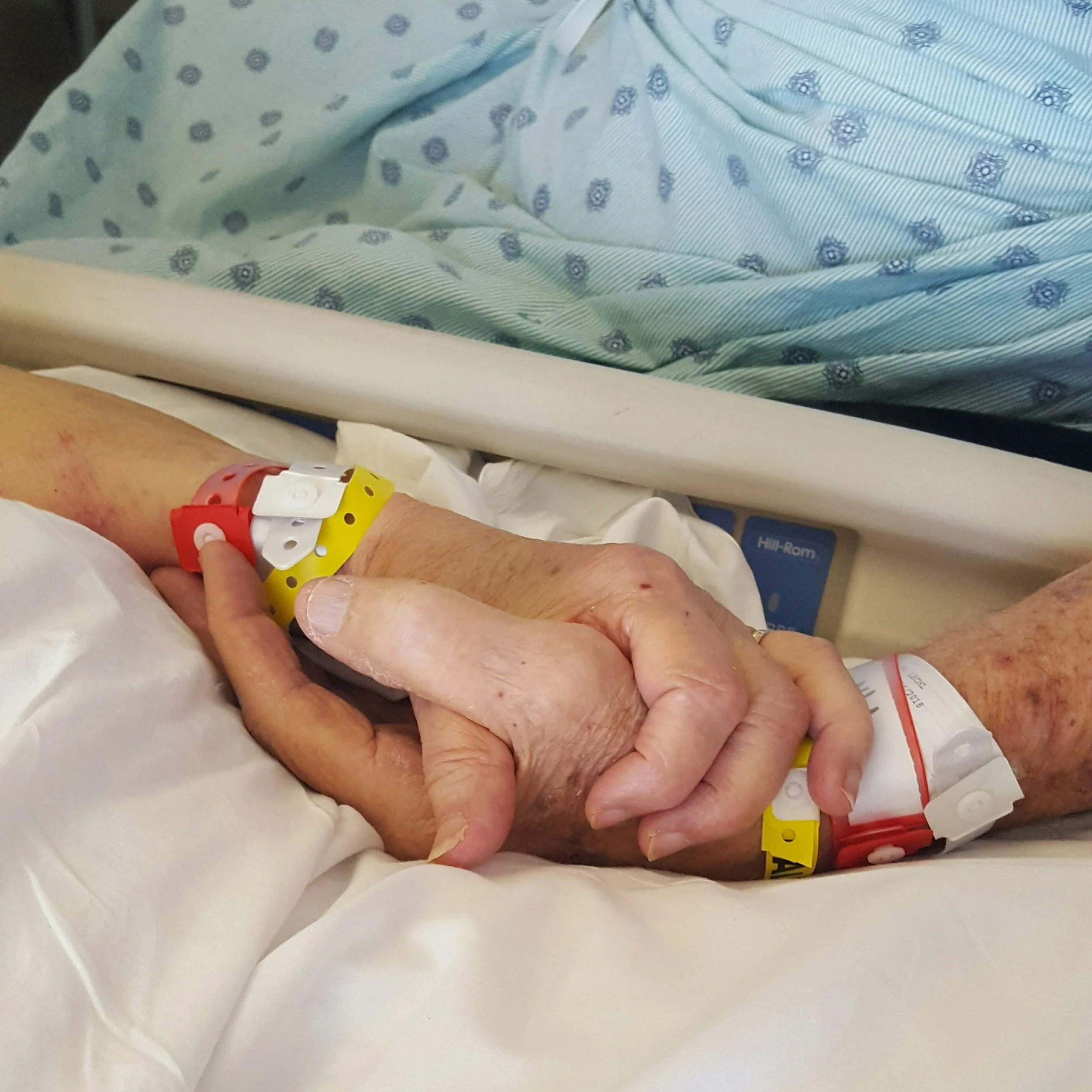

“Is This Safe?” Navigating the emotions behind dysphagia management
Learn why pursuing "zero risk" in dysphagia management can actually increase patient harm. This guide helps SLPs navigate family guilt, reframe aspiration risk, and align clinical recommendations with quality-of-life goals.

Wet Vocal Quality? Or is your ear playing tricks on you?
Is a wet vocal quality a reliable indicator of aspiration? Explore why relying on "gurgly" phonation during a clinical swallow evaluation can lead to unnecessary diet restrictions and why instrumental studies like VFSS are essential for dysphagia accuracy.

Strict NPO: Is It Doing More Harm Than Good?
Is Strict NPO doing more harm than good? Explore the ethical and clinical dilemma of dysphagia management. Learn about muscle atrophy, dry mouth, oral care, and alternatives to NPO status.

Dysphagia: What We Know, What We Don't Know, and What We Do From Here
Dysphagia research has gaps, but for SLPs, this is an opportunity, not a dead end. Explore the knowns—from essential oral care and swallowing exercises to the necessity of instrumental assessments (MBSS/FEES)—and the many unknowns in dysphagia management. Learn how to stay curious, collaborate, and creatively push the boundaries of evidence-based practice when the research is lacking.

Videofluoroscopy: How to ensure your study is more than just a snapshot
Transform your dysphagia practice. Learn why videofluoroscopy (VFSS/MBSS), demands standardized scoring (PAS, DIGEST, MBSImP) and advanced kinematic tools to overcome diagnostic gaps. This article details how moving beyond the 'practiced eye' and advocating for clinical standards elevates VFSS from an experienced guess to a truly objective, indispensable diagnostic tool for SLPs.

Treat the Patient, Not the Illness: An SLP's Stance on Temporary Dysphagia
When a 70-year-old patient has acute dysphagia, is a feeding tube the only choice? Read more to discover the high-stakes clinical dilemma of differentiating reversible, acute dysphagia (caused by sepsis/delirium) from long-term deficits. Learn the "Chicken or the Egg" principle and why resisting fear-based decisions saved this patient's independence.

A Case Study of Aspiration: What would you do?
Aspiration doesn't always mean NPO. Learn to distinguish harmless micro-aspiration from true pathological risk by analyzing patient factors like COPD, mobility, and cognition. Stop the fear. Read more!
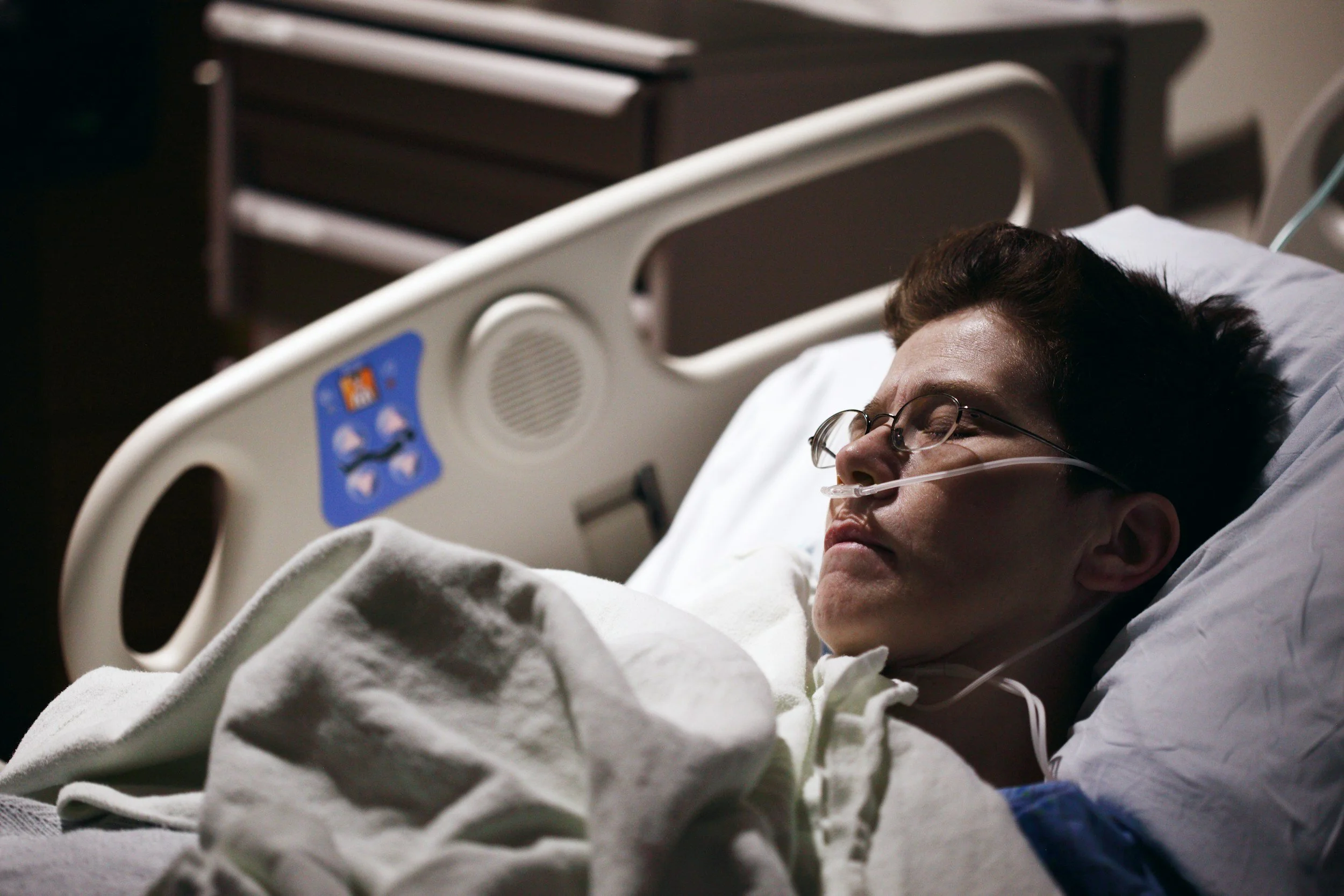
From Sustaining Life to Honoring It: Redefining the SLP’s Role in End-of-Life Care
As an SLP, what do you do when traditional rehab goals (restore, recover) no longer apply? This article tackles the most difficult ethical dilemma in end of life care. Learn the crucial difference between Hospice, Palliative Care, and Rehabilitation. Discover how to shift your focus from sustaining life to honoring it by using an evidence-based, palliative approach to swallowing and nutrition. Master the communication tools needed to guide families toward comfort, dignity, and making choices that truly align with the patient’s final wishes.

Over-treatment in Dysphagia: Why Less is More
Essentialist SLP: Stop Over-Treating Dysphagia. Learn to cut through the clinical chaos and complex protocols to focus on the 'vital few' interventions that truly improve patient outcomes and quality of life. This deep dive challenges the efficacy of thickened liquids and examines the ethical use of feeding tubes in complex cases like late-stage Alzheimer's.